US Flu Season Wanes but Child Death Toll Mounts at 139
The 2025-26 US flu season is receding, but 139 children have died — 85% unvaccinated — as Trump nominates a new CDC director.
Overview
The 2025-26 United States influenza season is entering its final weeks, with surveillance data indicating that transmission rates are declining across most regions. But the epidemiological record left behind is sobering. As of mid-April 2026, the season has claimed the lives of 139 children — a toll that public health officials at the Centers for Disease Control and Prevention (CDC) warn reflects a persistent and preventable gap in pediatric vaccination coverage. The waning of seasonal flu does not diminish the significance of these losses, nor the structural vulnerabilities they reveal. Against this backdrop, the Trump administration has nominated a new leader for the CDC, injecting fresh uncertainty — and some grounds for cautious optimism — into the federal public health apparatus at a sensitive moment.
Current Situation
 Image: Pexels/Negative Space
Image: Pexels/Negative Space
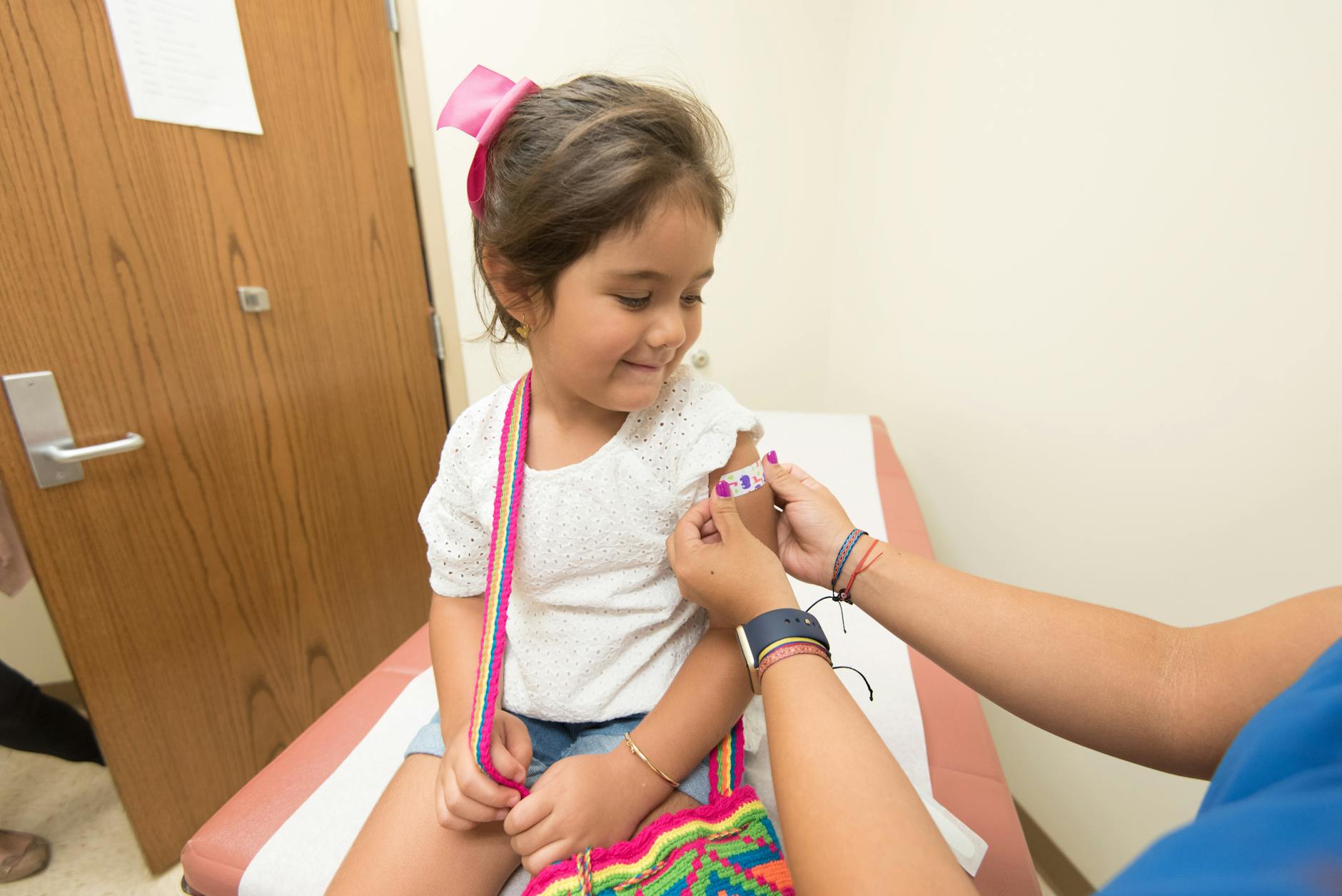
The most recent reporting period added 12 more pediatric deaths to the season’s cumulative count, bringing the total to 139 child fatalities attributable to influenza in the 2025-26 season, according to CIDRAP (the Center for Infectious Disease Research and Policy at the University of Minnesota), which tracks CDC data. Pediatric influenza deaths are among the few influenza-related fatalities subject to mandatory reporting in the United States, making this figure one of the more reliable indicators of the season’s true severity at the household level.
Of those deaths where vaccination status was known, approximately 85% of children who died had not received an influenza vaccine this season. This statistic carries significant weight: it is not a marginal association but a dominant pattern, reinforcing years of clinical evidence that seasonal influenza vaccination substantially reduces the risk of severe outcomes in children. It does not mean vaccination guarantees protection — influenza vaccines carry variable efficacy depending on strain match — but the scale of the disparity is difficult to set aside as coincidental.
Adult mortality data, as is typical, runs on a longer lag and is estimated rather than counted directly. Seasonal influenza kills tens of thousands of Americans in an average year across all age groups, with the elderly and immunocompromised carrying the heaviest burden. The 2025-26 season appears to have tracked broadly within historical ranges for severity, though final burden estimates will not be available until the CDC publishes its end-of-season report later this year.
The trend line, at least, is moving in the right direction. Influenza-like illness (ILI) rates and laboratory-confirmed positive test percentages have both declined across multiple consecutive weeks, consistent with the late-season pattern typical of northern hemisphere flu cycles. Most regions are reporting low or minimal activity.
Affected Regions
Influenza activity during the 2025-26 season followed a broadly national spread, with no single region escaping transmission entirely. The United States experiences influenza as an endemic-to-epidemic seasonal phenomenon rather than a geographically isolated outbreak, meaning the affected population is effectively the entire country — roughly 335 million people — with heterogeneous risk based on age, health status, and vaccination coverage.
Pediatric deaths, while occurring nationwide, tend to cluster in communities and demographic groups with lower vaccination uptake. Rural areas, regions with limited access to primary care, and populations where vaccine hesitancy has gained cultural traction have historically seen disproportionate pediatric flu mortality. The CDC’s FluView surveillance system tracks regional ILI trends week by week; at this writing, the South and parts of the Midwest were among the last areas to see activity fully decline, consistent with prior seasonal patterns.
No new geographic spread beyond the continental United States is being reported in connection with the domestic 2025-26 season. This is a nationally circulating strain, not a novel pathogen.
Risk Assessment
 Image: Pexels/Speak Media Uganda
Image: Pexels/Speak Media Uganda
Seasonal influenza remains one of the highest-burden respiratory pathogens in the United States on an annual basis, and the 2025-26 season does not appear to represent a departure from that baseline. The 139 pediatric deaths recorded so far do not, on their own, signal an unusually severe season by historical standards — prior years have seen totals ranging from under 100 to over 200 — but they reinforce that even an “average” flu season exacts a measurable human cost.
The vaccination gap is the central risk factor. With roughly 85% of pediatric flu deaths occurring in unvaccinated children, the data make a direct case that unvaccinated children represent the population most acutely at risk from preventable influenza mortality. Infants under six months of age, who are too young to be vaccinated directly, depend on household and community immunity for protection — a dynamic that makes vaccination of older children and adults in their orbit a matter of indirect but real consequence.
Children with underlying medical conditions — including asthma, neurological disorders, and obesity — face elevated risk of severe influenza complications regardless of vaccination status, though vaccination continues to offer meaningful protection in these groups as well. The CDC’s Advisory Committee on Immunization Practices (ACIP) recommends annual influenza vaccination for everyone aged six months and older, with no exceptions for otherwise healthy individuals.
The transition in CDC leadership introduces a secondary layer of institutional risk. Federal public health agencies play a coordinating and norm-setting role in vaccination campaigns; prolonged leadership vacancies or sharp directional changes in messaging can affect how state and local health departments calibrate their public outreach.
Prevention & Response
On April 16, 2026, the Trump administration announced the nomination of Erica Schwartz, a former deputy surgeon general of the United States, to serve as the next director of the CDC, according to CIDRAP. If confirmed, Schwartz would bring direct federal public health experience to the role — her prior work includes authoring Coast Guard policy on pandemic influenza and other viral disease outbreaks, suggesting familiarity with the operational and planning dimensions of large-scale infectious disease response.
The nomination comes during an active period of restructuring within the Department of Health and Human Services, which oversees the CDC. Public health observers have noted that the agency’s communications posture and budget outlook have both been subject to revision in recent months. A confirmed director with a background in emergency preparedness and outbreak policy would, at minimum, provide a degree of institutional continuity in those areas.
For the current flu season, the primary prevention lever — vaccination — has already largely played out. The window for influenza vaccination in the 2025-26 season is effectively closed as the virus recedes. The public health focus now appropriately shifts toward end-of-season analysis: evaluating vaccine effectiveness for the strains that circulated, identifying coverage gaps that contributed to pediatric deaths, and informing the composition and distribution strategy for the 2026-27 vaccine.
Annual influenza vaccination remains the single most evidence-supported intervention available to the general public. The CDC and the World Health Organization both maintain that routine vaccination of eligible individuals is the foundation of community-level influenza protection. For parents and caregivers, the actionable takeaway ahead of next season is straightforward: schedule vaccination for all eligible household members — including children — before the 2026-27 flu season begins, ideally in early autumn before peak transmission.
Antiviral medications such as oseltamivir (Tamiflu) remain available by prescription for treatment of active influenza infection, particularly for high-risk individuals, and can reduce the duration and severity of illness when initiated early. These are not substitutes for vaccination but remain a meaningful clinical tool during active infection.
The United States enters the inter-season period with its public health infrastructure in a state of active transition. How effectively the incoming CDC leadership can consolidate vaccine messaging, rebuild public trust in routine immunization, and prepare the country for the next respiratory virus season will be among the defining public health questions of the year ahead.
Sources
- CIDRAP — “US flu season receding but still deadly, with 12 more child deaths” (April 10, 2026): https://www.cidrap.umn.edu/influenza-general/us-flu-season-receding-still-deadly-12-more-child-deaths
- CIDRAP — “Trump nominates Erica Schwartz, former deputy surgeon general, to head CDC” (April 16, 2026): https://www.cidrap.umn.edu/public-health/trump-nominates-erica-schwartz-former-deputy-surgeon-general-head-cdc