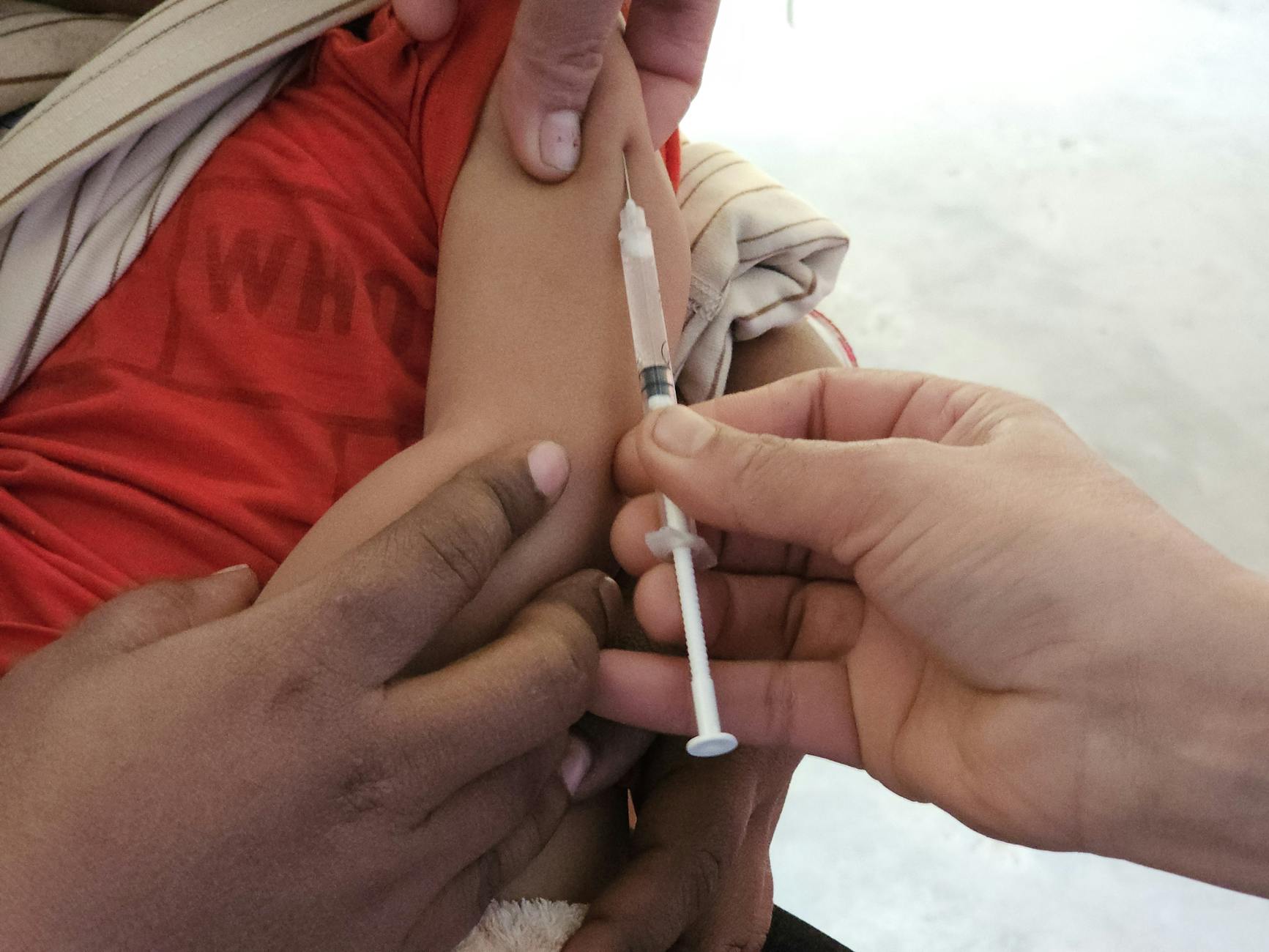
Measles Surges Across Bangladesh and the United States
Bangladesh reports 19,161 suspected measles cases and 166 deaths in one month; US cases near 1,800 as South Carolina closes its largest outbreak in 35 years.
Overview
Measles — a vaccine-preventable disease that the world came within reach of eliminating — is staging a serious resurgence on two continents simultaneously. In Bangladesh, a nationwide outbreak declared in early April 2026 has swept through nearly the entire country within weeks, killing scores of young children. In the United States, cumulative case counts are approaching levels not seen since before modern vaccination programs took hold, following a run of linked outbreaks across multiple states. The convergence of these events — in a high-density lower-middle-income country and in one of the world’s wealthiest nations — underlines a shared vulnerability: wherever vaccination coverage erodes, measles returns quickly and punishes hardest those who are youngest.
Current Situation
 Image: Pexels/gorden murah surabaya
Image: Pexels/gorden murah surabaya
According to a WHO Disease Outbreak Notification published on 23 April 2026, Bangladeshi health authorities reported 19,161 suspected measles cases and 2,897 laboratory-confirmed cases between 15 March and 14 April 2026 — a single-month window. Within that period, 166 measles-related deaths were recorded, yielding a case fatality rate (CFR) of approximately 0.9%. That figure is consistent with expected CFRs in settings where children are malnourished or lack access to supportive care, and where vitamin A deficiency is prevalent. The burden falls overwhelmingly on the youngest: 79% of reported cases involve children under five years of age, the cohort most vulnerable to severe complications including pneumonia, encephalitis, and death.
In the United States, the trajectory is different in character but not in direction. The Center for Infectious Disease Research and Policy (CIDRAP) reported at the end of April that total US measles cases were approaching 1,800 — a figure that would represent one of the worst years in recent American history. South Carolina, which bore the brunt of the domestic surge, formally closed its outbreak with 997 confirmed cases, a tally that CIDRAP describes as the largest single US outbreak in 35 years. New cases continued to emerge in Utah and Arizona as that report was published, indicating that transmission had not been fully interrupted across the country. Guatemala was also noted by CIDRAP as experiencing pediatric measles deaths in the same reporting period, suggesting that the Western Hemisphere’s momentum toward measles elimination has stalled at multiple points simultaneously.
Affected Regions
Bangladesh’s outbreak is geographically vast by any measure. Of the country’s 64 administrative districts, 58 are now affected, spanning all eight administrative divisions. That breadth points to a systemic gap in population immunity rather than a localized failure of surveillance or response — measles does not spread this widely this fast unless substantial pockets of unvaccinated or under-vaccinated children exist across an entire national geography. Dhaka, Chattogram, and other densely populated urban divisions are presumed to be among the highest-burden areas given their population concentrations, though the WHO notification does not disaggregate district-level case counts at this stage.
In the US, the geographic pattern reflects a different dynamic: outbreaks seeded within close-knit communities with concentrated vaccine hesitancy, then spreading along social networks. South Carolina’s cluster, now closed, was the epicenter of domestic transmission. Active spread in Utah and Arizona suggests that the outbreak has not been fully contained by that state’s closure — the virus is finding new susceptible populations in neighboring regions. A notable technical development from Cook County, Illinois adds a further dimension: CIDRAP reported that a single measles infection was detected in that jurisdiction using untargeted ultra-deep metagenomic sequencing of wastewater — a technique that requires no prior knowledge of which pathogen to look for. Public health officials described the finding as a potential template for passive community surveillance, capable of flagging infections before clinical cases are reported.
Risk Assessment
 Image: Pexels/Asad Photo Maldives
Image: Pexels/Asad Photo Maldives
WHO assessed the Bangladesh outbreak as a significant public health event warranting immediate international attention under the International Health Regulations (IHR) framework, which triggered the formal disease outbreak notification process. The risk within Bangladesh is rated high given the scale of spread, the age distribution of cases, and the mortality already recorded. The international risk is assessed as lower but not negligible: Bangladesh has extensive labour migration patterns and cross-border movement with India and Myanmar, and measles is transmissible enough — with a basic reproduction number (R₀) typically between 12 and 18 in unvaccinated populations — that border controls have limited efficacy against airborne spread.
The concentration of deaths among children under five in both Bangladesh and Guatemala serves as the clearest signal that vaccination coverage gaps are now translating directly into preventable child mortality.In the United States, the risk calculus differs. Severe outcomes and deaths remain rare by comparison, owing to generally higher baseline health status and access to supportive care. However, the US situation carries its own structural risk: concentrated communities with low vaccination uptake can sustain transmission indefinitely once introduced, and the political environment around childhood immunisation has grown more contested. Congressional hearings in late April saw Robert F. Kennedy Jr., in his capacity as Secretary of Health and Human Services, deny responsibility for the measles resurgence despite his long record of public anti-vaccine advocacy. His nominee for CDC director, Erica Schwartz, was described in testimony as someone who would act independently — a characterisation that public health observers noted is difficult to reconcile with the removal of longstanding CDC vaccine promotion infrastructure under the current administration.
The European Centre for Disease Prevention and Control (ECDC) included measles in its Week 16 Communicable Disease Threats Report for 12–18 April 2026, flagging it alongside Zika and chikungunya as active threats requiring monitoring in EU and EEA member states. While Europe has not reported outbreak-level transmission comparable to Bangladesh or the US, the ECDC’s inclusion of measles reflects ongoing vigilance about importation risks from regions with active circulation.
Prevention & Response
Bangladesh’s emergency response moved quickly following the official WHO notification. A targeted measles-rubella (MR) vaccination campaign launched on 5 April 2026 — the day after the IHR focal point notified WHO — targeting children in affected districts. Nationwide surveillance has been strengthened to improve case detection and ensure that confirmed and suspected cases are being captured and reported consistently. Epidemiological teams are conducting active case-finding and contact tracing in priority districts. WHO and partner organisations are supporting the government response, though the scale of the outbreak — nearly 20,000 suspected cases across 58 districts within a single month — will test both logistical and human resource capacity.
In the United States, the formal public health response has continued through state health departments. South Carolina’s outbreak closure reflects successful interruption of transmission chains, achieved through targeted vaccination, case isolation, and contact tracing within affected communities. The wastewater surveillance finding in Cook County, while representing only a single detected infection, has drawn attention from public health researchers as a model for passive early-warning systems — particularly for diseases like measles where a single case in an under-vaccinated community can seed a cluster within days.
For travellers and clinicians, the practical guidance remains consistent with longstanding recommendations: verify measles-mumps-rubella (MMR) vaccination status before travel to any country with active circulation. Two doses of MMR vaccine confer approximately 97% protection against measles infection. Infants too young for routine vaccination (under 12 months in most schedules) can receive an early dose before travel if the exposure risk is elevated — parents should consult their healthcare provider. Any febrile illness with rash following travel to Bangladesh or other outbreak-affected countries should prompt immediate notification of local public health authorities, and affected individuals should avoid healthcare settings and crowded spaces while awaiting assessment.
Sources
- WHO Disease Outbreak News – Measles, Bangladesh (DON598), 23 April 2026: who.int
- CIDRAP – Measles case counts mount in Utah, Arizona, while Bangladesh, Guatemala battle deadly outbreaks, 1 May 2026: cidrap.umn.edu
- CIDRAP – South Carolina measles outbreak ends as US cases near 1,800, 27 April 2026: cidrap.umn.edu
- CIDRAP – Detection of measles via wastewater surveillance, Cook County, Illinois, 30 April 2026: cidrap.umn.edu
- CIDRAP – In hearings, RFK Jr claims no responsibility for measles spread, 22 April 2026: cidrap.umn.edu
- ECDC – Communicable Disease Threats Report, Week 16, 12–18 April 2026: ecdc.europa.eu
Sources
- WHO Disease Outbreak News – Measles, Bangladesh (DON598) ↗
- CIDRAP – Measles case counts mount in Utah, Arizona, while Bangladesh, Guatemala battle deadly outbreaks ↗
- CIDRAP – South Carolina measles outbreak ends as US cases near 1,800 ↗
- CIDRAP – Detection of measles via wastewater surveillance, Cook County, Illinois ↗
- CIDRAP – In hearings, RFK Jr claims no responsibility for measles spread ↗
- ECDC Communicable Disease Threats Report, Week 16, 2026 ↗