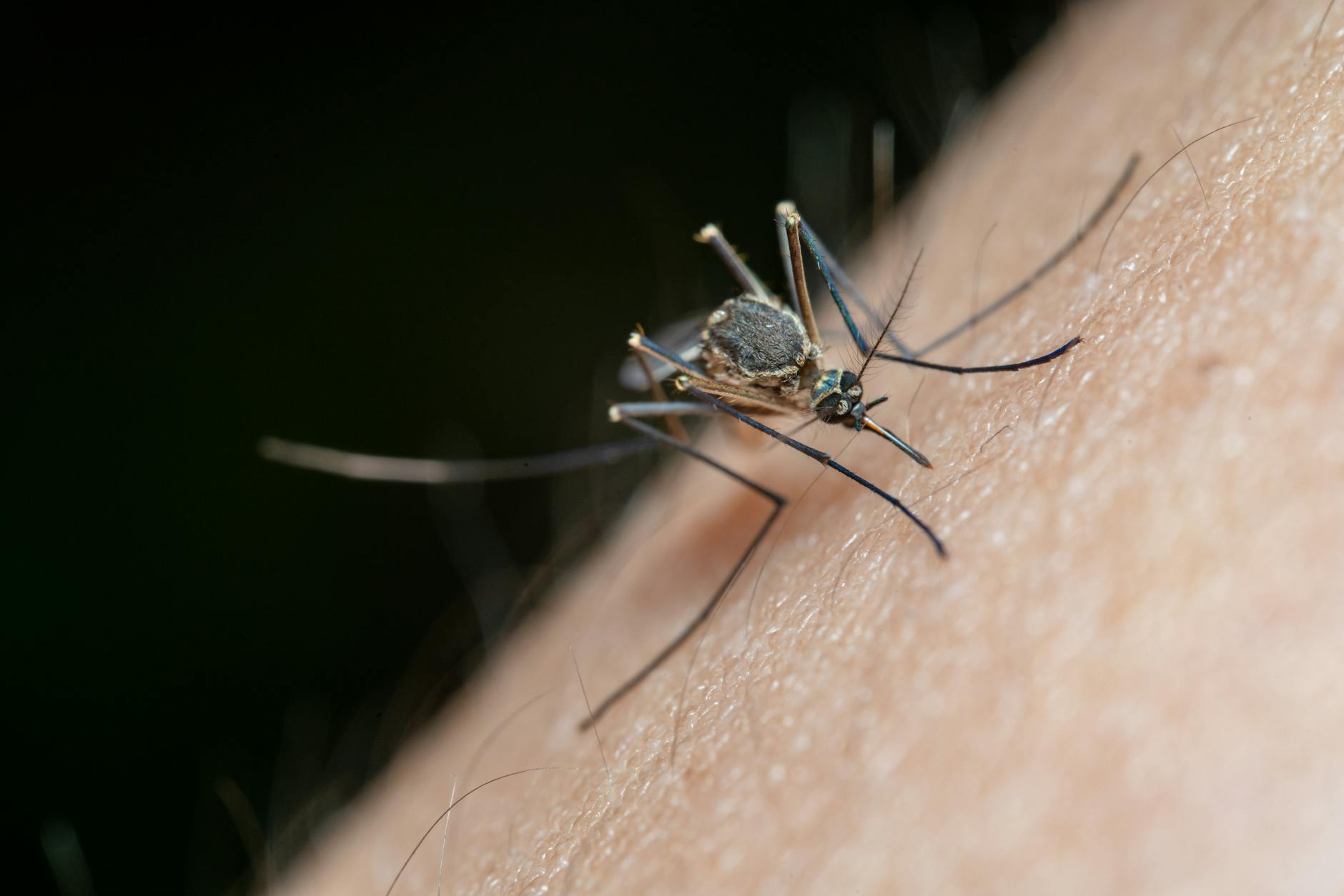
Dengue Fever Maintains Elevated Global Transmission in Early 2026
Dengue fever continues to spread across tropical and subtropical regions globally, with ECDC tracking elevated transmission levels into early 2026.
Overview
Dengue fever remains one of the most geographically expansive and rapidly growing vector-borne diseases on the planet. As of the European Centre for Disease Prevention and Control (ECDC)‘s most recent monthly epidemiological overview, published 30 March 2026, global dengue transmission continues at elevated levels across a wide arc of tropical and subtropical nations. Unlike many infectious disease crises that spike and recede within defined epidemic windows, dengue now behaves as a near-permanent fixture of the global disease burden — with annual case totals consistently dwarfing those recorded just a decade ago.
The disease is caused by any one of four antigenically distinct serotypes of the dengue virus (DENV-1 through DENV-4), all transmitted primarily by the Aedes aegypti mosquito and, to a lesser degree, Aedes albopictus. This biological complexity means that immunity to one serotype provides no lasting protection against the others — and a second infection with a different serotype substantially raises the risk of severe dengue, the life-threatening form of the disease.
The ECDC’s Communicable Diseases Threat Report, issued weekly and synthesized monthly for dengue specifically, aggregates surveillance data from national health ministries, the World Health Organization (WHO), and regional health networks worldwide. It represents one of the most comprehensive real-time windows available into global dengue dynamics.
Current Situation
 Image: Pexels/gorden murah surabaya
Image: Pexels/gorden murah surabaya
The ECDC’s March 2026 dengue overview arrives on the heels of a year — 2025 — in which global dengue notifications exceeded historical averages in multiple regions simultaneously. The WHO reported that 2023 had already been a record year with more than 6.5 million cases registered globally, a figure that subsequent years have continued to challenge. Preliminary surveillance data compiled by the ECDC for the first quarter of 2026 suggests transmission has not entered any meaningful seasonal trough in the Southern Hemisphere, where countries in South America and Southeast Asia are moving through or past their typical peak dengue season.
Crucially, the proportion of cases that progress to severe dengue — characterised by plasma leakage, severe bleeding, and organ impairment — remains a concern in settings where health system capacity is strained. Case fatality rates for severe dengue can range from below 1% in well-resourced clinical environments to as high as 5% or more where advanced supportive care is unavailable. The ECDC tracking does not provide a single global fatality figure given the uneven quality of death attribution data across reporting countries, but national authorities in several high-burden nations have recorded mortality upticks alongside elevated caseloads.
One of the most epidemiologically significant trends is the expanded co-circulation of multiple serotypes in the same geographic areas. When DENV-3 or DENV-4 re-enters a population that has been exposed predominantly to DENV-1 or DENV-2 in prior seasons, the proportion of individuals facing a secondary heterotypic infection — and thus elevated severe disease risk — increases. ECDC surveillance has flagged this serotype shift as a driver of severity in several recent outbreaks.
Affected Regions
Dengue’s global footprint now spans more than 100 countries. The Americas have experienced a dramatic and sustained rise in caseloads since 2023, led by Brazil, which alone has accounted for the majority of the Western Hemisphere’s reported cases in recent years. Colombia, Argentina, Peru, and several Caribbean nations have also recorded significant transmission. In South America, the seasonality of dengue roughly mirrors the austral summer, meaning that early 2026 falls within or just past the peak transmission window.
In Southeast Asia, countries including Bangladesh, Thailand, Vietnam, the Philippines, and Malaysia continue to report active transmission. India, with its vast population and diverse Aedes mosquito habitats across both urban and rural settings, contributes substantially to regional and global totals. Sri Lanka, historically prone to large cyclical outbreaks, remains under active surveillance.
Europe is no longer immune to locally acquired dengue transmission: Italy, France, and Spain have each recorded autochthonous cases in recent years, driven by the establishment of Aedes albopictus (the tiger mosquito) across Mediterranean coastal areas.Sub-Saharan Africa remains a region of significant concern due to underreporting. Dengue circulates broadly across West and East Africa, but weak diagnostic infrastructure means confirmed case counts represent only a fraction of true burden. The ECDC highlights Africa as a region where surveillance gaps complicate accurate global risk assessments.
Risk Assessment
 Image: Pexels/Igud Supian
Image: Pexels/Igud Supian
The WHO currently classifies dengue as a “neglected tropical disease” with pandemic potential, a designation that reflects both its extraordinary global burden and the structural neglect it receives relative to diseases with higher political profiles. From an epidemiological standpoint, several intersecting factors are driving the sustained global expansion.
Urbanisation is foremost among them. Aedes aegypti is a highly peridomestic mosquito — it breeds in small, stagnant water containers in and around human dwellings, thrives in dense urban environments, and has adapted effectively to informal settlement conditions where water storage practices and waste management are inconsistent. As tropical and subtropical cities grow, they become increasingly hospitable mosquito habitats.
Climate change is compounding this dynamic. Rising average temperatures and shifting precipitation patterns are expanding the geographic range of Aedes mosquitoes into higher altitudes and latitudes that were historically inhospitable. This means previously non-endemic areas — including parts of southern Europe and higher-elevation zones in the Americas and Asia — face a genuine and growing risk of endemic establishment.
Vulnerable populations include infants and young children in endemic areas (who often experience their first serotype exposure), travellers returning from endemic regions (who may seed local transmission in low-endemic countries with competent vector populations), and immunocompromised individuals. Pregnant women with dengue face elevated risks of adverse birth outcomes, including preterm delivery and foetal distress.
The ECDC’s risk assessment for EU/EEA residents emphasises imported cases as the dominant risk pathway, with locally acquired transmission confined to Mediterranean coastal regions during summer months when Ae. albopictus is active.
Prevention & Response
The global public health response to dengue operates on two parallel tracks: vector control and, increasingly, vaccination.
Vector control remains the foundation of dengue prevention programmes worldwide. This encompasses environmental management (eliminating standing water breeding sites), insecticide-based interventions (larviciding and adulticiding), and community-level education campaigns. The WHO’s Global Vector Control Response framework, adopted in 2017, provides the strategic architecture for these efforts, though implementation quality varies widely by country.
On the vaccine front, the dengue landscape has grown more complex and more hopeful in recent years. Dengvaxia (CYD-TDV), developed by Sanofi Pasteur, was the first licensed dengue vaccine but carries a critical caveat: it is recommended only for individuals with prior dengue infection, as seronegative recipients face elevated severe disease risk from vaccination. This limitation has constrained its public health utility in contexts where pre-vaccination serostatus testing is impractical.
More recently, Qdenga (TAK-003), developed by Takeda, has received regulatory approval in multiple countries and the EU. It does not carry the same serostatus restriction as Dengvaxia and has demonstrated meaningful efficacy across serotypes in clinical trial settings. Several endemic countries are evaluating or piloting Qdenga as part of routine childhood immunisation programmes, which could represent a meaningful shift in the long-term trajectory of dengue burden.
The ECDC continues to issue its monthly dengue worldwide overview as part of its Communicable Diseases Threat Report series — a resource that serves as an essential surveillance reference for EU member state health authorities, travel medicine practitioners, and international outbreak response teams. The monthly cadence reflects the reality that dengue is not an episodic emergency but an ongoing, dynamic global health challenge requiring sustained institutional attention.
For travellers, standard precautions remain relevant year-round in endemic regions: repellent use (DEET or picaridin-based), protective clothing during peak mosquito activity periods (dawn and dusk), and accommodation in air-conditioned or screened environments where feasible. Clinicians should maintain dengue in the differential diagnosis for febrile returning travellers from any tropical or subtropical destination.
Sources
- European Centre for Disease Prevention and Control (ECDC) — Dengue Worldwide Overview (monthly), 30 March 2026. https://www.ecdc.europa.eu/en/dengue-monthly
- World Health Organization (WHO) — Dengue and Severe Dengue Fact Sheet. https://www.who.int/news-room/fact-sheets/detail/dengue-and-severe-dengue